A 63-year-old African-American female presented on 6/1/17 for a podiatry consultation at the local hospital with dry gangrene on the first, second and third toes on her right foot. She said she noticed her toes turning black after having her toenails debrided a couple weeks beforehand. The patient described sharp pain in the right foot as 10 out of 10 on the visual analogue scale. The pain was localized to the distal right foot.
The patient’s comorbidities included type 2 diabetes, peripheral arterial disease (PAD), end-stage renal disease (ESRD), gastroparesis, gastroesophageal reflux disease (GERD) and glaucoma. She had no known drug allergies and was taking Humulin 70/30, metoprolol tartrate (Lopressor, Novartis Pharmaceuticals), verapamil 120 mg, omeprazole, and gabapentin. The patient acknowledged being a former smoker and denied recreational drug use. She noted a family history of prostate cancer from her father and breast cancer from her mother. The patient’s past surgical history included a previous fistula on her arm.
Upon examination on 6/1/17, the patient’s vital signs included a temperature of 98.10F, heart rate of 71 beats per minute, a respiratory rate of 18, and a blood oxygen level of 96 percent. Her pertinent lab test results included a white blood cell count of 8.0 K/uL, creatine of .17 mg/dL, and hemoglobin A1C of 8.6 percent. The patient was alert and oriented to time, place and event.
Her neurovascular evaluation revealed non-palpable dorsalis pedis and posterior tibial pulses bilaterally. Light touch detection was absent on the soles of her feet. Dermatologically, the patient had dry, stable-appearing gangrene of the first, second and third toes on her right foot. A musculoskeletal exam revealed hypersensitivity upon palpation of the right forefoot.
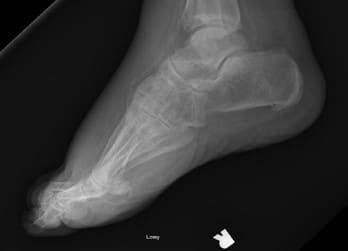
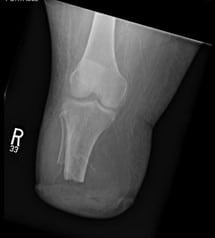
Radiographic images of the right foot showed no evidence of osteomyelitis or soft tissue emphysema. There was severe calcification of the pedal arteries (see Figure 1).
Figure 1
Arterial Doppler waveforms and segmental pressures were obtained for both lower extremities. There was no obtainable ankle-brachial index (ABI) measurement secondary to severe arterial calcification. Doppler waveform analysis alone suggested evidence of multilevel disease with severe distal ischemia to the right foot.
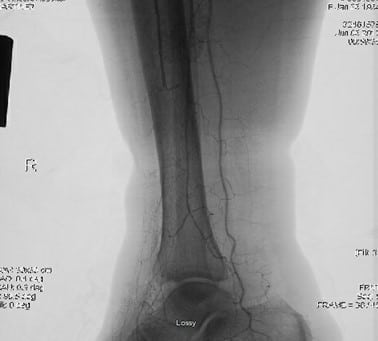
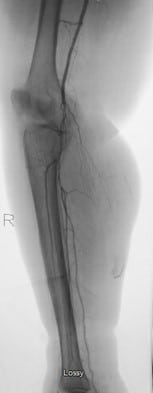
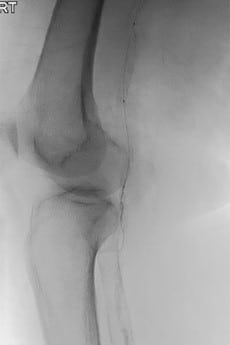
The patient was subsequently referred for a vascular consult. Performing an arteriogram on 6/6/2017, vascular surgeons noted right popliteal artery and tibial vessel disease below the knee. On 6/9/2017, the patient had a right leg arteriogram (see Figures 2-5). Employing orbital atherectomy and balloon angioplasty, the vascular surgery team successfully restored in-line flow to the foot from the posterior tibial and peroneal arteries. However, the anterior tibial artery was occluded at the mid-tibia level. The vascular surgeons indicated that the patient should be able to heal a transmetatarsal amputation (TMA).
Raising Concerns About Potential Non-Healing of a TMA
Despite the vascular intervention, the podiatry service had ongoing concerns for the ability of this patient to heal a TMA procedure. She had no blood flow to the dorsal flap as the anterior tibial artery was completely occluded at the mid-tibia level. Accordingly, we ordered transcutaneous oxygen (TCPO2) measurements that revealed 7 mmHg in the forefoot, 9 mmHg at the ankle level, 44 mmHg below the knee and 98 mmHg above the knee.
In our discussion of treatment options with the patient and her daughter, we emphasized that a below-knee amputation (BKA) offered the most predictable level for spontaneous healing. We discussed how a TCPO2 of 7 mmHg indicated extremely poor perfusion to the foot. However, the patient and her daughter refused a BKA and wanted to try a TMA. After surgical consultation with the family about the poor prognosis for limb salvage, the patient signed the consent form and was brought to the operating room (OR).
Prior to making the incision, we made one last attempt to evaluate perfusion to the dorsal and plantar flaps of the right foot and utilized the SPY Elite Fluorescence Imaging (Stryker). Once the patient was on the OR table, indocyanine green (IG) dye was injected into her IV and this was followed by a 10 ml saline flush. The OR lights were dimmed, and attention was directed to the monitor, which showed a region of poor perfusion on the dorsal flap. However, the plantar flap had a more robust uptake of the IG dye, which gave us a little more optimism that a TMA was worth trying.
Escalating Postoperative Concerns
We performed the TMA procedure on 6/12/17 and the patient had some early dusky changes to the dorsal lateral aspect of the incision line on the first post-op day. On the fourth post-op day, we decided to remove the sutures where the duskiness was noted to avoid further compromise to the flap.
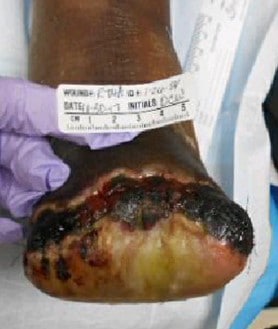
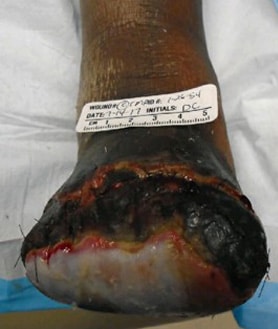
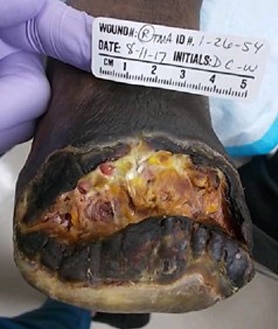
The patient was discharged from the hospital and had follow-up care at a wound healing center. Hyperbaric oxygen (HBOT) was started on 7/10/17 once her chest X-ray and echocardiogram were free of any pathology. Unfortunately, her amputation stump proceeded to necrosis over the next several weeks (see Figures 6-8).
The patient had a difficult postoperative period and was readmitted to the hospital several times due to other medical complications such as diabetic ketoacidosis, encephalopathy and nausea related to her gastroparesis. This led to missed post-op visits. On 8/11/17, the patient and her daughter accepted the need for a BKA, and she was admitted for orthopedic surgery consultation. She had the BKA on 8/17/17 once vascular surgery notified the orthopedic surgeon that she should be able to heal the BKA level.
During the postoperative period, the patient was readmitted to the hospital on 9/4/17 due to severe pain at the BKA amputation stump. Radiographs of the surgical site were negative for any osseous pathology or soft tissue emphysema (see Figure 9). On 9/7/17, all sutures were removed from the amputation site as there was full healing at that time without complication.
Figure 9
Sadly, this patient passed away more than three months later on 12/22/17.
Final Notes
This case study shows that even with a multispecialty approach to limb salvage, there can still be failure to save a patient’s limb. Even with the restoration of two vessel run-off to her foot and the use of HBOT, the patient’s limb was ultimately not salvageable. It is likely this patient was diagnosed with occlusive PAD much too late in her life to provide her with a good chance at limb salvage. Furthermore, she had extensive comorbidities with ESRD and PAD significantly reducing the possibility of successful limb salvage. This particular case teaches the importance of giving the patient and family members realistic expectations for limb salvage when taking into account the patient’s comorbidities and vascular studies.
Dr. Patel is a fourth-year student at the Dr. William M. Scholl College of Podiatric Medicine at the Rosalind Franklin University of Medicine and Science.
Dr. Stuart is the Clinic Director of the Ascension St. Vincent Hospital Podiatry Residency Program in Indianapolis. He is board-certified by the American Board of Podiatric Surgery and the American Board of Wound Management.