In a case study of a patient with idiopathic progressive neuropathy, gout, bilateral cavus deformities and a 30-year history of tobacco use, these authors discuss the use of split-thickness skin grafting to facilitate healing of a transmetatarsal amputation wound.
In comparison to types of cancer, the five-year mortality rate following a major (proximal to ankle) lower extremity amputation (56.6 percent) is second only to lung cancer (80 percent).1,2 In fact, even for a minor amputation (distal to the ankle), including toes and metatarsals, the mortality rate at five years is 46.2 percent.2 Furthermore, in many cases involving severe infection and/or significant tissue loss, primary closure may not be feasible, and open amputation is required. In these cases, long-term planning and selection of appropriate wound care modalities, along with skilled nursing care, physical therapy, proper offloading, and medical management, are critical for ultimately achieving ulcer- and amputation-free days.
Although many good options exist for advanced topical wound care therapies, skin grafting remains one of the most reliable and effective means of achieving wound closure in patients with difficult-to-heal ulcers and amputations.3 In a recent meta-analysis, Yammine and Assi evaluated the outcomes of split-thickness skin grafting (STSG) on diabetic lower extremity ulcers.4 Based on their review of 11 studies involving a total of 757 patients with 759 lower extremity ulcers, they found that STSG is “the ideal method to treat non-infected recurrent or recalcitrant ulcers of the leg and dorsal foot.”
Accordingly, let us take a closer look at a recent case involving the use of negative pressure wound therapy (NPWT) and STSG to help heal an open transmetatarsal amputation (TMA) secondary to severe infection in a patient with a history of peripheral neuropathy and a severe cavus foot deformity.
The 63-year-old male patient initially presented with a severe infection of a chronic plantar forefoot and sub-first metatarsal ulcer on the right foot. The physical exam revealed diffuse erythema, edema and warmth surrounding the ulcer site. There was purulent drainage from the ulcer site, and it was easy to visualize the bone.
He had a history of idiopathic progressive neuropathy affecting both lower extremities, gout, hypertension, bilateral anterior pes cavus deformity, and multiple non-healing ulcers on both feet. The patient did not have diabetes but acknowledged being a former tobacco user for over 30 years. Previous treatments for the patient’s ulcer included topical wound care dressings, oral and intravenous antibiotics, and hyperbaric oxygen therapy (HBOT). Offloading was extremely difficult given the bilateral foot ulcers, and the patient’s role as primary caregiver for a sick family member who required transportation several times per week to medical facilities.
The patient was admitted to the hospital and had a TMA that day. Given the extent of infection in the adjacent forefoot and the size of the plantar ulcer, a decision was made to perform an open amputation at the mid-shaft level of the metatarsals. Antibiotic cement beads were applied to the site and removed at the first post-operative dressing change. We initiated the use of NPWT, and this continued following hospital discharge. The amputation site appeared clean, and the patient was discharged on a short course of cephalexin.
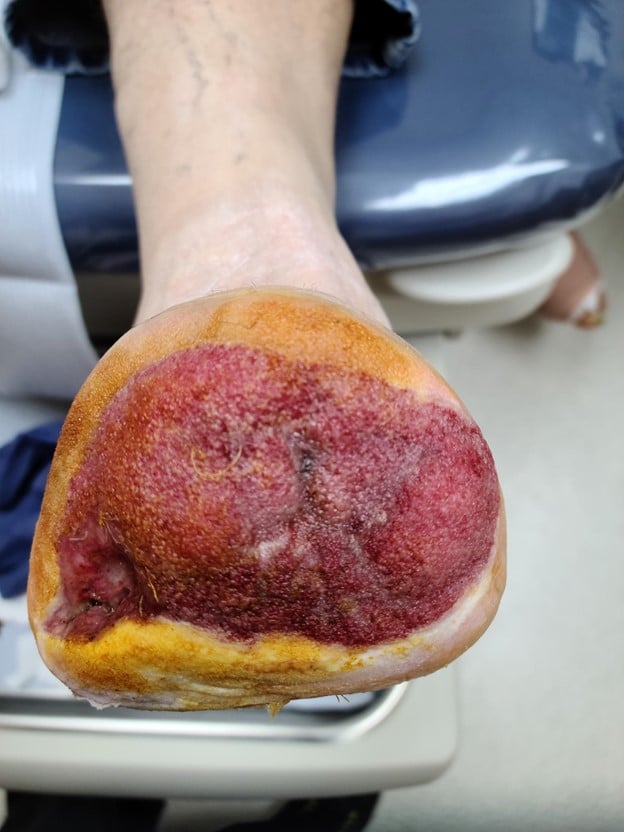
Over the next 12 weeks, the patient received NPWT and the amputation site continued to decrease in size with increased granulation tissue noted (see Figure 1). At this point, he was referred to the vascular surgeon for skin grafting.
Figure 1
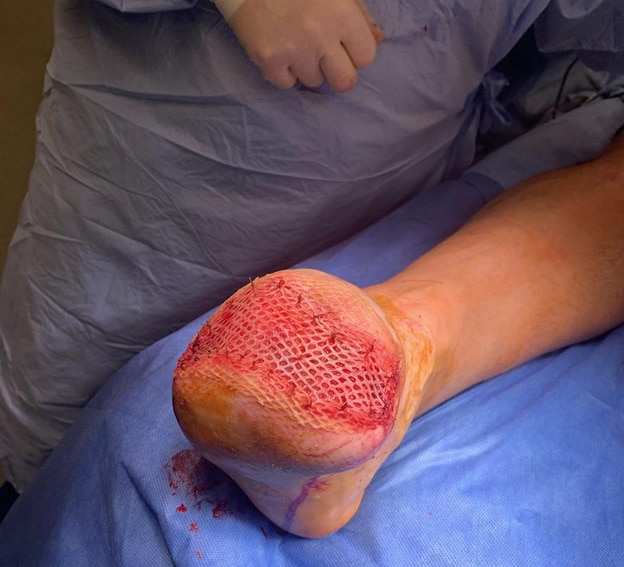
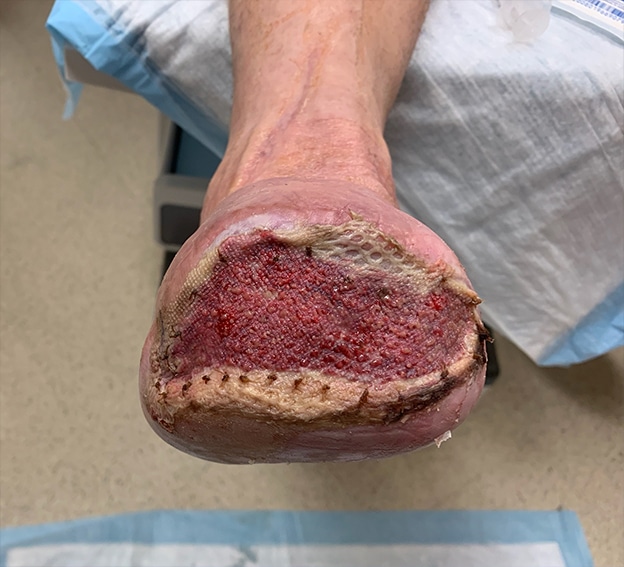
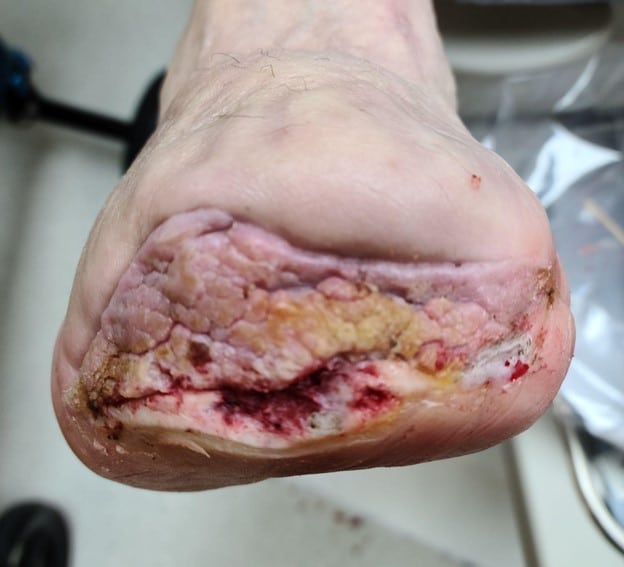
The patient had a STSG (see Figure 2) and there was subsequent application of a portable NPWT system the patient had previously been using at home as a bolster dressing. It is important to note that this allowed the patient to be discharged on the same day of surgery. On the fifth postoperative day following the skin grafting, the NWPT dressing was removed. There was excellent take of the graft (see Figure 3). The amputation site was nearly completely epithelialized six weeks after the STSG procedure (see Figure 4).
Final Notes
Despite a growing number of currently available advanced wound care modalities, STSG remains an effective and reliable option for obtaining wound closure in complex cases, including open amputation sites. In this case study, the patient was managed primarily by members of the toe and flow team (podiatric and vascular surgery) at different institutions and geographic locations. However, the team members were able to follow the patient through a common electronic medical record (EMR) system and close communication. This case represents a good example of how the multidisciplinary approach for limb preservation can extend beyond the walls of a hospital or office setting and result in a positive outcome.
Dr. Isaac is the Director of Research with Foot & Ankle Specialists of the Mid-Atlantic.
Dr. Hicks is an Associate Professor in the Department of Vascular Surgery and Endovascular Therapy at the Johns Hopkins University School of Medicine in Baltimore.
References
1. Armstrong DG, Swerdlow MA, Armstrong AA, Conte MS, Padula WV, Bus SA. Five year mortality and direct costs of care for people with diabetic foot complications are comparable to cancer. J Foot Ankle Res. 2020;13(1):16.
2. Barshes NR, Sigireddi M, Wrobel JS, et al. The system of care for the diabetic foot: objectives, outcomes, and opportunities. Diabet Foot Ankle. 2013 Oct 10;4. doi: 10.3402/dfa.v4i0.21847.
3. Rose JF, Giovinco N, Mills JL, Najafi B, Pappalardo J, Armstrong DG. Split-thickness skin grafting the high-risk diabetic foot. J Vasc Surg. 2014;59(6):1657-63.
4. Yammine K, Assi C. A meta-analysis of the outcomes of split-thickness skin graft on diabetic leg and foot ulcers. Int J Low Extrem Wounds. 2019;18(1):23-30.