Preventing an initially requested below-knee amputation to avoid prolonged wound care, these authors discuss the multidisciplinary workup and successful limb salvage procedures for a patient presenting with an infected TMA site and advanced chronic limb-threatening ischemia.
The health-care burden imposed by chronic limb-threatening ischemia (CLTI) cannot be overstated. Reportedly over 2 million people in the United States have CLTI and are at high risk for major amputation with mortality approaching 50 percent at five years.1,2 The utilization of a multidisciplinary limb salvage team, via the “toe and flow” model, has demonstrated superior results in wound healing and limb salvage in patients with CLTI.3-6
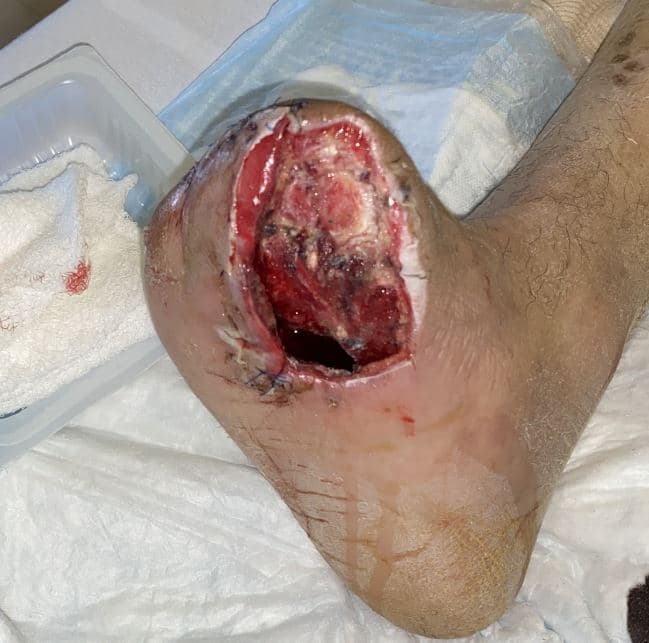
Accordingly, we share a case of successful limb salvage for a patient who presented with a WIFi stage IV (Wound 3, Ischemia 3, Foot infection 2) infected transmetatarsal amputation (TMA).4 The 52-year-old male patient’s medical history included hypertension, type 2 diabetes mellitus and severe peripheral neuropathy. He had been traveling through California for the past few months and presented with an infected TMA that was previously performed at an outside facility.
Figure 1
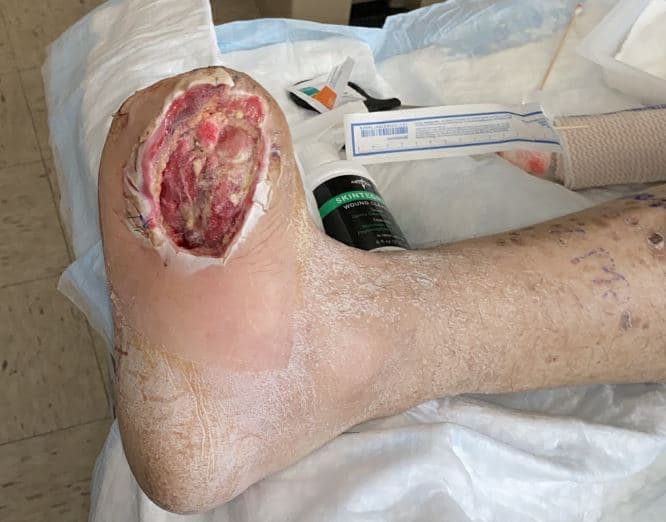
The patient had no prior history of vascular intervention and did not have routine medical care. He was admitted for medical optimization of his diabetes. The podiatry service evaluated the patient and performed urgent debridement. Non-invasive vascular labs revealed non-compressible ankle-brachial indices (ABIs) and an ultrasound demonstrated superficial femoral artery (SFA) and popliteal occlusion as well as monophasic tibial flow. Serial wound debridement allowed for source control and a healthy granulating wound bed. However, a large tissue defect presented a significant clinical challenge.
Figure 2
Initially, the patient desired a below-knee amputation to obviate the need for long-term wound care as this presented a burden that was not conducive to his living situation. Our limb salvage team approached him with the option for revascularization and a definitive Chopart’s amputation, which would allow discharge from the hospital with minimal wound care and expedited healing.
An angiogram revealed an occlusion of the SFA, popliteal and tibioperoneal trunk with reconstitution of the posterior tibial and peroneal arteries. Given the patient’s age, extensive disease burden and tissue loss, and difficulties with health-care access, we made a team decision to proceed with a femoral to posterior tibial bypass with great saphenous vein followed by a definitive Chopart’s amputation. Four days after surgery, the patient was discharged to our on-site acute rehabilitation facility where he was closely monitored and initiated physical therapy and gait exercises to allow for safe non-weightbearing mobility of his right leg.
He was able to follow up with our team for surveillance and had his sutures removed at three weeks post-op with complete healing of all his surgical incisions and no wound dehiscence.
Figure 3
The patient’s social situation required his return to New York, which presented a long-term clinical follow-up challenge for this high-risk patient. Fortunately, we were able to transition the patient to a well-established limb salvage program at a local hospital in the Bronx, N.Y., so he could continue to receive comprehensive follow-up care by both podiatric and vascular surgeons. At the patient’s six-week post-op visit with the New York team, duplex surveillance showed a widely patent bypass graft, there was complete healing of his Chopart’s amputation, and the patient was ambulating independently with no issues.
This case highlights the advanced stage of wound and disease presentation that we see in most underserved patients with CLTI. It also demonstrates the clinical challenges of long-term surveillance in these high-risk patients. Having a well-established limb salvage team allows for comprehensive decision making that can provide a treatment plan best tailored to the patient’s needs. Anatomic revascularization and amputation providing a functional limb can lead to a patient’s ability to return to society and thrive.
Additionally, with the Society of Vascular Surgery (SVS) and the American Podiatric Medical Association (APMA) working collaboratively and the increased reach of social networking, this case demonstrates that patients can be connected with multidisciplinary limb salvage teams across the country to provide comprehensive care irrespective of location.
Dr. O’Banion is an Assistant Clinical Professor of Surgery at the University of California San Francisco-Fresno. She is a Fellow of the American College of Surgeons and the Society for Vascular Surgery.
Dr. Oseni-Olalemi is a Clinical Associate at Valley Foot and Ankle Specialty Providers. She is board-certified by the American Board of Podiatric Medicine and is a member of the APMA.
Dr. Rivera is an Assistant Professor in the Department of Cardiothoracic and Vascular Surgery at the Albert Einstein College of Medicine. He is the Associate Chief of Vascular Surgery at Jacobi Medical Center. He is a Fellow of the American College of Surgeons and the Society for Vascular Surgery.
References
1. Duff S, Mafilios MS, Bhounsule P, Hasegawa JT. The burden of critical limb ischemia: a review of recent literature. Vasc Health Risk Manag. 2019;15:187-208.
2. Conte MS, Bradbury AW, Kolh P, et al. Global vascular guidelines on the management of chronic limb-threatening ischemia. J Vasc Surg. 2019;69(6S):3S-125S.e40.
3. Gabel J, Bianchi C, Possagnoli I, et al. Multidisciplinary approach achieves limb salvage without revascularization in patients with mild to moderate ischemia and tissue loss. J Vasc Surg. 2020;71(6):2073-2080.e1
4. Mills JL, Sr., Conte MS, Armstrong DG, et al. The Society for Vascular Surgery Lower Extremity Threatened Limb Classification System: risk stratification based on wound, ischemia, and foot infection (WIfI). J Vasc Surg. 2014;59(1):220-34 e1-2.
5. Armstrong DG, Conte MS, Rogers LC, Mills JL. The offspring of Sisyphus: steady progress in the decade since the “toe and flow” JAPMA-JVS special issue on limb preservation. J Am Podiatr Med Assoc. 2021;20-137. doi: 10.7547/20-137. Online ahead of print.
6. Rogers LC, Andros G, Caporusso J, Harkless LB, Mills JL, Sr., Armstrong DG. Toe and flow: essential components and structure of the amputation prevention team. J Am Podiatr Med Assoc. 2010;100(5):342-8.